EKG Rhythm Strips 51

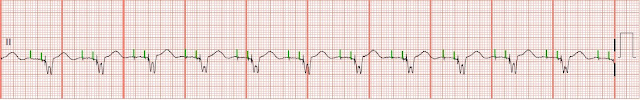
Identify the following rhythm strips. 1. 2. 3. 4. 5. Answers 1. Atrial fibrillation with unifocal PVCs The rhythm is irregular with some PVCs. The rate is 100/min. No P waves are present. Some fibrillatory activity is seen between the QRS complexes. It looks like there might be P waves present before the 5th complex and following but this appears to be part of the ST segment. If you look at the 1st complex you will see that following the T wave there is a slight depression followed by a slight positive rise. This appears to be repeated in the complexes that follows giving the impression that a P wave is present. The increase in the heart rate and shortening of the R-R interval would also give the impression that P waves are present. Two unifocal PVCs are seen. PR: ---, QRS: .12 sec, QT: .38 sec. The bottom tracing is an arterial blood pressure waveform. You can seen the hemodynamic effects of the PVCs on the arteria